Stellate Ganglion Blocks
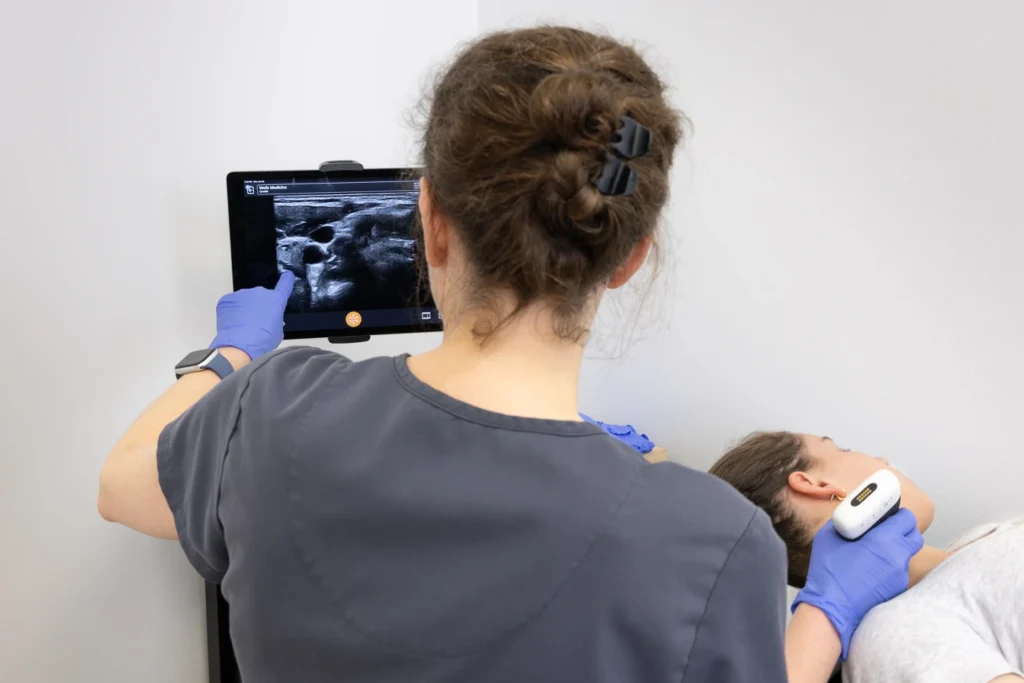
- The procedure involves an ultrasound-guided injection of long-acting anesthetic near a nerve cluster – the stellate ganglion – in the neck.
- The procedure itself typically takes less than 30 minutes and patients should be able to resume their normal daily activities immediately after.
- You may return for a second appointment on a subsequent day: Many patients experience significant relief from the block on one side only. Some will benefit after a block on the other side. The best likelihood of significant and durable results comes from blocks on both sides.
- You can return for maintenance treatments as needed – with some patients receiving significant relief from even a single treatment, and others returning periodically.
- Modulation of Sympathetic Nervous System: The stellate ganglion is a part of the sympathetic nervous system, which is involved in the body’s “fight, freeze, or flight” response. By blocking the activity of the stellate ganglion, SGB may reduce sympathetic nervous system hyperactivity observed in individuals with PTSD. This can lead to decreased arousal, anxiety, and alleviation of other PTSD symptoms.
- Alteration of Neurotransmitter Levels: SGB may influence the levels of neurotransmitters involved in PTSD. By modulating the release or activity of these neurotransmitters, SGB could potentially alleviate PTSD symptoms such as hyperarousal and intrusive thoughts.
- Normalization of Brain Activity: Functional imaging studies have shown abnormal activity in certain brain regions, such as the amygdala and prefrontal cortex, in individuals with PTSD. SGB may help normalize this activity by modulating neural circuits involved in fear processing and emotional regulation. Although we don’t have a verified pathway for how this happens yet.
- Reduction of Neuroinflammation: There is evidence to suggest that neuroinflammation plays a role in the pathophysiology of PTSD. SGB may have anti-inflammatory effects, leading to reduced neuroinflammation and improvement in PTSD symptoms.
- Enhancement of Fear Extinction: Fear extinction is the process by which learned fear responses are diminished over time. SGB may enhance fear extinction by modulating synaptic plasticity mechanisms in the brain, facilitating the extinction of traumatic memories and reducing the severity of PTSD symptoms. This is facilitated by therapy in the days and weeks after a SGB.
Overall, while the exact mechanisms of action are still being elucidated, SGB appears to exert its therapeutic effects on PTSD through a combination of neurobiological and physiological mechanisms.
- Rapid relief: Many patients experience immediate or significant pain and PTSD symptom reduction following the procedure. The effects can be both immediate and profound, offering a window of relief that has been described as transformative by many patients.
- Minimally invasive: SGB is performed on an outpatient basis, minimizing downtime and discomfort. Usually the right side SGB is enough for PTSD relief, but occasionally both sides need to be blocked for the best effects and a left side SGB can be done a day or two after the right side for increased effectiveness.
- Enhanced quality of life: By managing pain and PTSD effectively, SGB empowers individuals to regain functionality and enjoy daily activities. Relief often lasts several weeks to months.
- Innovative Approach: At the forefront of medical science, SGB offers hope where traditional treatments may have failed.
- Versatility: Effective for a range of conditions, including PTSD, anxiety disorders, and various types of chronic pain.
- PTSD / Post-traumatic stress disorder
- Severe anxiety
- CRPS / Complex regional pain syndrome of the upper extremity
- Vasoplegia of the upper extremity, or Raynaud’s syndrome
- Phantom limb pain of the upper extremity
- PHN / Postherpetic neuralgia that affects the head, face, chest, or neck
- Traumatic brain injury
- Long COVID